The application of the 'open' Hasson blunt troacar insertion technique to the pediatric patients
K. Karavdic*, N. Dziho, A. Jonuzi, A. Firdus, E. Milisic, A. Karamustafic
Clinic for Pediatric Surgery, Clinic Center of University Sarajevo, Bosnia and Herzegovina
Abstract
Introduction: There are several methods of creating pneumoperitoneum in patients who are planned to be subjected under laparoscopy procedure. The most commonly used method is generally a Veress needle insertion. In pediatric population treatment, the popular method is open blunt trocar insertion technique.
Objective: To describe the safety and efficacy of open laparoscopic access for the primary trocar using Hasson’s technique for pediatric laparoscopic surgery.
Methods: All 229 laparoscopic procedures that were performed at the Clinic for Pediatric Surgery Clinical Center of University Sarajevo between 2015.-2020. With Hasson’s technique were evaluated. Patients were aged from 6 months to 18 years.
Results: Most patients who had open laparoscopic access during the study period had diagnosis of acute appendicitis (n=165), impalpable undescended testicles (n=18), gallstones (n=17), varicocele (n=4), hernias (n=4) and other reasons (n=18). Three children had minor operative complications (2 cases of pre-peritoneal placement of trocar, which were recognized and corrected immediately and the other had omental bleeding). Two children had post-operative complications related to primary access (one port infection and other port site hematoma). Access to the abdominal cavity was generally accomplished in 3-12 minutes (average 4+2). Clinic follow-up ranged from 3-14 months.
Conclusion: Open laparoscopic access using modified Hasson’s technique was associated with no major or life-threatening complications. Hasson’s technique for the primary trocar for accessing the abdominal cavity is a safe and effective method and is recommended for all laparoscopic procedures in children.
Introduction
Access into the abdomen is one of the biggest challenges in pediatric surgery1. The first step of laparoscopic procedure is creating of the pneumoperitoneum and it is a step of the utmost importance. Pneumperitoneum creation is correlated with injuries to the gastrointestinal organs and large blood vessels. Half of the major complications happen prior to beginning of the surgery. Injuries of the large blood vessels in laparoscopic procedures is 2 in 10000 procedures. Number of more serious complications that are connected with mortality happens in 3.3 per 1000002. Main goal should be right decision of using a safe entry technique. At last, there is no general agreement on optimal method of entry into the peritoneal cavity.
There are two methods for creating a pneumoperitoneum, the classic closed technique (Veress needle) and open classic technique (Hasson technique)3 are the common most procedures used in laparoscopy for entry into the peritoneal cavity. Blind insertion of the Veress needle and of the first trocar is a significant cause of complications during laparoscopic surgery.
Open laparoscopic technique was first brought by Dr. Harrith Hasson from Chicago, who published a paper on this technique in the American Journal of Obstetrics and Gynecology in 1971. Hasson, in 2000., published review of 29 years of his laparoscopic experience. During that period, he did 5284 operations and proved entry technique to be safe and effective. He noted only 27 complications in this group of patients, the most of them having infected wounds and hematomas. Only one case of bowel perforation as a consequence of port entry was noted4.
Objective
The aim of this article is to report the results of our experience with usage of the open technique in laparoscopic surgery and to evaluate the time taken and complications.
Methods
All 229 cases that were operated at Clinic for Pediatric Surgery Clinical Center of University Sarajevo between years 2015 and 2020 were taken into consideration in evaluation of using this technique presented in this article. They were aged from 6 months to 18 years.
We described the experience and complications in children who had primary access by Hasson’s technique. A small transverse or semicircular incision approximately 5 to 10 mm is made in the inferior umbilical fold. (Figure 1) Subcutaneous tissue is dissected, (Figure 2) the skin edges are retracted with small Langenbeck retractors and the subcutaneous fat tissue separated from the umbilical scar till the linea alba and the rectus sheath is visualized. (Figure 3) 2/0 or 3/0 polyglactin purse-string sutures (vicryl) are inserted on either side of the midline. (Figure 4) Both supporting seems are pulled up to make a bridge-like elevation of rectus. Rectus sheath is incised in the midline through both the line and peritoneum close to the umbilicus where all layers of the abdominal wall are adjoining. Blunt trocar-cannula (5-10mm) should be inserted in the first port after visualizing the intra-peritoneal viscera. The suture is then secured around the gas inlet site of the primary cannula so that it secures it wouldn’t be pulled out of the abdomen by accident. The cannula is fixed to the abdominal wall with a silk suture to prevent air leakage. After the carbon dioxide has been insufflated, the optical equipment is introduced in the usual way. The creation of pneumoperitoneum is faster and uniform with the open laparoscopic technique. The port site is closed in layers after suturing the rectus with non-absorbable sutures.
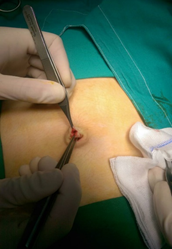
Figure 1: A small transverse or semicircular incision
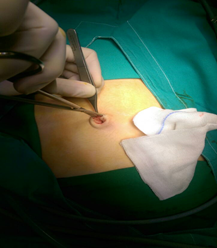
Figure 2: Subcutaneous tissue is dissected approximately 5 mm to 10mm is made in the inferior umbilical fold approximately 5mm to 10mm
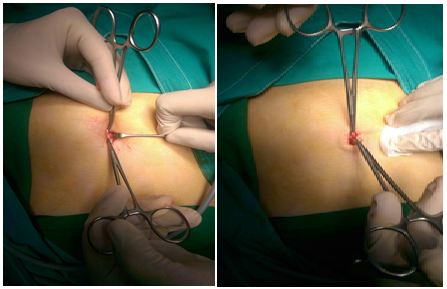
Figure (3,4): the skin edges are retracted with small Langenbeck retractors and the fat tissue separated from the umbilical scar till the linea alba and the rectus sheath is visualized
Results
All 229 laparoscopic procedures performed at Clinic for Pediatric Surgery Clinical Center of University Sarajevo between years 2015 and 2020 using Hasson’s technique were evaluated. Patients were aged from 6 months to 18 years. 132 (57.64%) of the patients were boys and 97 (42.36%) of them were girls. (diagram 1). The average age of the patient was 10.86 years.
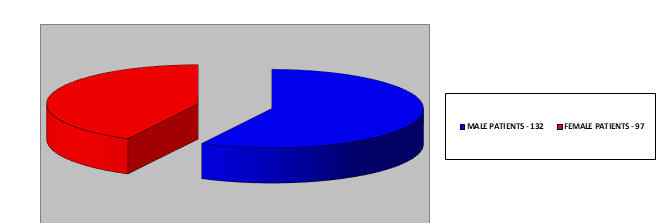
Diagram 1: Representation of percentage rate of male/female ratio
Most patients who had open laparoscopic access during the study period had diagnosis of acute appendicitis (n=165), impalpable undescended testicles (n=18), gallstones (n=17), varicocele (n=4), hernias (n=4) and others reasons (n=18). (diagram 2)
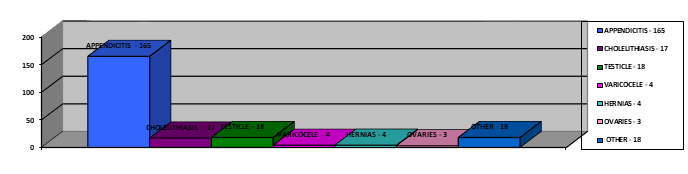
Diagram 2: Representation of individual operative procedures
Three children had minor operative complications (2 cases of pre-peritoneal placement of trocar, which were recognized and corrected immediately and the other one had omental bleeding). Two children had post-operative complications related to primary access (one port infection and other port site hematoma). Access to the abdominal cavity was generally secured in 3-12 minutes (average 6). Clinical follow-up was ranged from 3-14 months.
The highest number of open Hasson techniques was in year 2018 and 2017 with over 50 patients. (diagram 3)
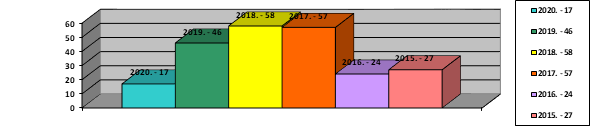
Diagram 3: Linear view of Hasson procedures shown accordngly by years
In patients treated for appendectomy and cholecystectomy, the first umbilical trocar was 10mm wide. This size was necessary to remove the appendix and gallbladder. In all other cases, the first, umbilical port was 5 mm wide in diameter. (diagram 4)
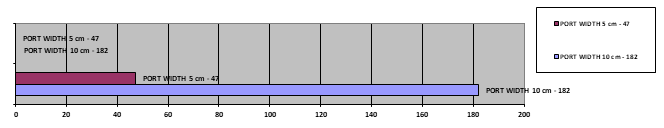
Diagram 4: Representation of operative procedures accordingly to the width of the used umbilical port – 10 cm and 5 cm
Twelve (5,24%) children had minor operative complications (2 cases of pre-peritoneal placement of trocar, which were recognized and corrected immediately and the other one had omental bleeding). Ten (4,37%) children had post-operative complications related to primary access (port infection), but none had umbilical hernia during 3 months of follow-up after surgery.
Access to the abdominal cavity was generally secured in 6 minutes (range 3 to 10). Clinical follow-up was ranged from 3-6 months.
Discussion
Open insertion with visualization of the abdominal cavity before introduction of the primary cannula reduces the risk of major visceral or vascular injury5. Open Hasson’s technique is popular among pediatric surgeons and is gaining popularity among adult surgeons6. According to the survey of the American Academy of Pediatrics (section of Urology), the technique used to obtain pneumoperitoneum was an important predictor of the complication rate7. The technique used by respondents included Veress needle technique to obtain pneumoperitoneum (45%), open (Hasson) technique only (33%) and both (23%). The Veress needle was associated with 2.6% rate of significant complications in contrast to a 1.2% serious complication rate for open technique (p<0.006). This difference between both techniques remained significant for experienced (more than 100 cases) pediatric urologists8. There is limited data available in children regarding the complications related to primary trocar insertion and is probably under-reported. The incidence of all complications in pediatric laparoscopic surgery was reported to be 2%10. Vascular or visceral injuries are the most devastating complications of laparoscopy.
One serious complication reported by Esposito was a vascular injury with bowel injury9. This was secondary to blind insertion of the first umbilical trocar. Valla reported laparoscopic bowel injuries ((0.5%) out of 3090 laparoscopic procedures) in children10. None were related to blind insertion of primary trocar suggesting the safety of open technique in experienced hands. Even with the open technique, inadvertent opening of the bowel had been reported in the literature9,11. Inadvertent bowel opening can occur if there is an area that is adherent to the abdominal due to the previous operations. However, with open technique, it would be easier to diagnose the resulting injury immediately and ensure its management without delay. We had no major complications during the placement of the first port in our 229 patients series. Minor complications include hematoma at site of trocar, subcutaneous emphysema infection, incisional hernia and omental or abdominal wall bleedings12. As in our experience, 2 pre-peritoneal placements of cannula had occurred at the beginning of the series. Infection of trocar wound (4,37%) is well known and is usually limited and is easily treated by antibiotics or drainage13. Incisional hernia is uncommon in children if proper closure of ports is achieved. In adults, hernia was reported at 3 mm port site14,15. The purse-string Hasson’s technique has several advantages. Even small gas leakage results in poor vision due to small abdominal cavity. The second advantage is easy fascial closure as the previous purse-string suture is tightened and has secured the fascia closure. In children, one unique problem is tenting of the peritoneum while inserting the port or Veress needle. This results from loose extraperitoneal fat attachment to the abdominal wall. This problem is encountered more in blind insertion of first trocar. Other problems include narrow peritoneal cavity that increases the risks to injure major, vessels or viscera.
A disadvantage of the open technique is more tissue dissection on the port site. This can result in minor risks of local hematoma and infection. Increasing number of surgeons performing open technique laparoscopy has not been widely adopted mainly due to gas leakage from the wound and because it is time-consuming. Injuries to underlying viscera and vessels by needles and trocars have been reported even when the open technique is used.
Primary access (open or blind) technique is sometimes difficult in obese children. This problem might be overcome in open Hasson’s technique by lifting the linea alba by small artery forceps and pulling it up at skin level. The fascia and peritoneum are subsequently incised individually. It is very important to assess the intra-abdominal length of the cannula over the abdominal wall before securing the purse-string suture.
There are 2 problems if the cannula is long: the cannula may obscure the view or damage intervening organs, as there is very little distance between the anterior and posterior abdominal wall in children. Recently the crescent-shape laceration of the transverse colon was reported by Hasson cannula in a lean built 29-year-old patient16,17. The cause of profuse bleeding was blunt injury to the middle colic artery. The time required to apply the modified Hasson’s technique, in our experience averaged 6 minutes. Surgeons preferring the closed technique usually argued that open technique was time consuming and it was frustrating to be lost in pre-peritoneal space. There clearly exists a learning curve during which pediatric surgeons gain a systemic approach to the procedure. Once the technique is mastered, rapid access is achieved as in our case. English literature review via Medline database showed limited reports of complications in children related to access for pneumoperitoneum. Multivariate analysis in adults showed that open Hasson’s technique was safer and resulted in fewer complications as compared to Veress needle insertion18. For pediatric laparoscopic surgery, there is no such comparison available in the literature to draw the definite conclusion. Multi-center controlled randomized trials are required in children using open or blind techniques to clearly demonstrate the benefits of either technique. Recently European association for endoscopic surgery suggested that available data on Veress needle and open access technique do not allow them to principally favor the use of either technique19.
Conclusion
Open laparoscopic access using Hasson’s technique was associated with no major or life-threatening complications.
Hasson’s technique for the primary trocar for accessing the abdominal cavity is a safe and effective method and is recommended for all laparoscopic procedures in children because a small risk of injury.
References
- Ahmad G, Duffy JM, Phillips K, et al. Laparoscopic entry techniques. Cochrane Database Syst Rev. 2008.
- Hasson HM. A modified instrument and method for laparoscopy. Am J Obstet Gynecol. 1971; 110(6): 886-87.
- Trocars: safety and selection. Emergency Care Research Institute. Health Devices. 1998; 27(11): 376-399.
- Hasson HM, Rotman C, Rana N, et al. Open laparoscopy: 29-year experience. Obstet Gynecol. 2000; 96(5 Pt 1): 763-766.
- Lal P, SingP L, Agarwal N, et al. Open Port Placement of the First Laparoscopic Port: A Safe Technique. Journal of the Society of Laparoendoscopic Surgeons. 2004; 8: 364–366.
- Zaraca F, Catarci M, Gossetti F, et al. Routine use of open laparoscopy 1006 consecutive cases. J Laparoendosc Adv Surg Tech A. 1999; 9: 75-80.
- Peter CA. Complications in pediatric urologic laparoscopy: Results of a survey. J Urol. 1996; 155: 1070-1073.
- Chen MK, Schropp KP, Lobe TE. Complications minimal access surgery in children. J Pediatr Surg. 1996; 31: 1161-1165.
- Esposite C, Ascione G, Garipoli V, et al. Complications of pediatric laparoscopic surgery. Surg Endosc. 1997; 11: 655-657.
- Valla JS, Trevino E, Demay A, et al. Laparoscopic bowel injuries in children. Pediatric Endosurgery and Innovative Technique. 2001; 5: 253-257.
- Hasson HM. Open laparoscopy: 29 years-experience. Obstet Gynecol. 2000; 96: 763-766.
- Bax NMA, Zee DC van der. Complications in laparoscopy in children. In: Bax NMA, Georgson DE, Najmaldin AS, Valla JS, editors. Endoscopic Surgery in children: Berlin: Springer-Verlag. 1999; 357-368.
- Hermans BP, Otte JB. Laparoscopic appendicectomy; pros & cons - literature review of 4190 cases. Acta Chir Belg. 1997; 97: 110-117.
- Bergemann JL, Hibbert ML, Harkins G, et al. Omental herniation through a 3-mm umbilical trocar site: unmasking a hidden umbilical hernia. J Laparoendosc Adv Surg Tech A. 2001; 11: 171-174.
- Voitk A, Rizoli S. Blunt Hasson trocar injury: long intra-abdominal trocar and lean patient - a dangerous combination. J Laparoendosc Adv Surg Tech A. 2001; 11: 259-262.
- Mayol J, Garcia-Aguilar J, Ortiz-Oshiro E, et al. Risks of the minimal access approach for laparoscopic surgery: Multivariate analysis of morbidity related to umbilical trocar insertion. World J Surg. 1997; 21: 529-533.
- Bonjer HJ, Hazebroek EJ, Kazemier G, et al. Open versus closed establishment of pneumoperitoneum in laparoscopic surgery. Br J Surg. 1997; 84: 599-602.
- Neudecker J, Sauerland S, Neugebauer E, et al. The European association for Endoscopic Surgery clinical practice guideline on the pneumoperitoneum for laparoscopic surgery. Surg Endosc. 2002; 16: 1121-1143.
- El Ghoneimi A, Valla JS, Limonne B, et al. Laparoscopic appendectomy in children: report of 1,379 cases. J Pediatr Surg. 1994; 29: 786-789.
